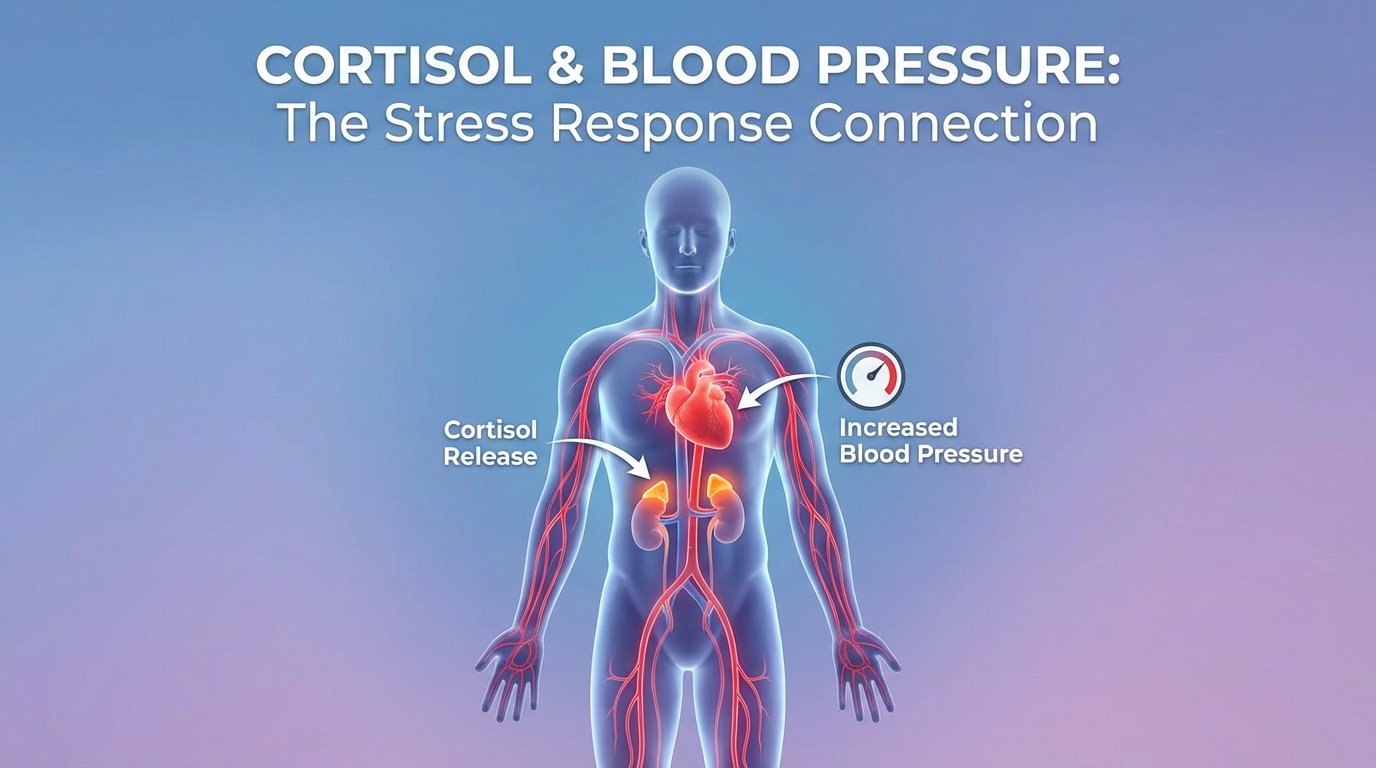
When you think about what raises blood pressure, diet, exercise, and genetics likely come to mind. But there is another powerful driver that often flies under the radar: cortisol, your body's primary stress hormone. Chronic elevation of cortisol does not just make you feel anxious or tired. It directly raises blood pressure, increases cardiovascular risk, and can lead to sustained hypertension.
Cortisol is produced by the adrenal glands and plays a vital role in your body's stress response. In short bursts, cortisol is helpful. It mobilizes energy, sharpens focus, and prepares your body to handle challenges. But when cortisol stays elevated for weeks, months, or years due to chronic stress, sleep deprivation, or medical conditions, it wreaks havoc on your cardiovascular system.
Research shows that even mild cortisol elevation within the "normal" range is linked to higher blood pressure and increased risk of heart attacks and strokes. For people with conditions like Cushing syndrome (a disorder of excessive cortisol production), high blood pressure is present in roughly 80% of cases.
This article will explain how cortisol affects blood pressure, the warning signs of elevated cortisol, how to test for cortisol excess, and evidence-based strategies to lower cortisol naturally. If you have high blood pressure and chronic stress, this connection may be one of the missing pieces in your blood pressure management puzzle.
How Cortisol Raises Blood Pressure
Cortisol influences blood pressure through several interconnected mechanisms. Understanding these pathways helps explain why managing stress and cortisol levels is critical for cardiovascular health.
1. Sodium Retention and Volume Expansion
Cortisol has mineralocorticoid activity, meaning it can mimic the effects of aldosterone, a hormone that tells your kidneys to hold onto sodium and water. When cortisol levels rise, sodium retention increases blood volume. More blood volume means more pressure against artery walls, directly raising blood pressure. Studies show that blood pressure increases are apparent within 24 hours of cortisol elevation and are accompanied by significant sodium retention.
2. Blood Vessel Constriction
Cortisol increases the responsiveness of blood vessels to other hormones like adrenaline and noradrenaline. These hormones cause blood vessels to constrict (narrow), which increases resistance to blood flow. Higher resistance means higher blood pressure. Cortisol also enhances the production of angiotensin II, a potent vasoconstrictor, further tightening blood vessels.
3. Reduced Nitric Oxide Production
Nitric oxide (NO) is a molecule that relaxes and widens blood vessels, helping to keep blood pressure low. Elevated cortisol reduces nitric oxide bioavailability, impairing the blood vessels' ability to dilate. This reduction in vasodilation contributes to sustained hypertension.
4. Sympathetic Nervous System Activation
Cortisol enhances activity in the sympathetic nervous system, the "fight or flight" branch of your nervous system. This increases heart rate and cardiac output (the amount of blood your heart pumps per minute) and raises blood pressure. Chronic sympathetic activation is a hallmark of stress-related hypertension.
Together, these mechanisms can raise systolic blood pressure by 5-15 mmHg in people with chronically elevated cortisol. For someone with already borderline hypertension, this can be enough to push them into the hypertensive range.
Cushing Syndrome: When Cortisol Goes Too High
Cushing syndrome is a rare but serious condition caused by prolonged exposure to high cortisol levels. It can result from a pituitary or adrenal tumor, long-term use of corticosteroid medications (like prednisone), or other medical conditions that overstimulate cortisol production.
About 80% of people with Cushing syndrome develop hypertension. Blood pressure elevation in Cushing syndrome is often difficult to control with standard medications and may not normalize until the underlying cause of cortisol excess is treated.
Common signs and symptoms of Cushing syndrome include:
- Rapid weight gain, especially in the face (moon face), neck (buffalo hump), and abdomen
- Purple or pink stretch marks (striae) on the abdomen, thighs, or arms
- Easy bruising and thin, fragile skin
- Muscle weakness, particularly in the shoulders and hips
- Fatigue and irritability
- High blood pressure and high blood sugar
- Irregular menstrual periods (in women) or erectile dysfunction (in men)
- Increased thirst and frequent urination
If you have high blood pressure plus several of these symptoms, mention them to your doctor. Early diagnosis and treatment of Cushing syndrome can reverse many of the complications, including hypertension. Left untreated, Cushing syndrome significantly increases the risk of heart disease, stroke, and diabetes.
Cortisol and Everyday Hypertension
You do not need to have Cushing syndrome for cortisol to affect your blood pressure. Chronic stress from work, relationships, financial worries, or sleep deprivation can keep cortisol levels moderately elevated for months or years. This subclinical cortisol elevation is far more common than Cushing syndrome and contributes to the development of hypertension in millions of people.
A 2023 study of over 400 adults found that individuals with high levels of stress hormones (including cortisol) detected in their urine were significantly more likely to develop high blood pressure over the next 6-7 years. Higher cortisol was also linked to an increased risk of cardiovascular events, including heart attack and stroke.
This finding highlights an important point: you do not need cortisol levels in the "abnormal" range to experience cardiovascular harm. Cortisol elevation within the high-normal range, driven by chronic stress, can still push your blood pressure up and increase long-term heart disease risk.
How to Test Cortisol Levels
Cortisol testing is straightforward and can be done using blood, saliva, or urine. Each method has specific uses and advantages.
Blood Cortisol Test
A blood test is the most common way to measure cortisol. Cortisol levels follow a circadian rhythm, peaking in the morning (typically between 6 AM and 8 AM) and dropping to their lowest point at night. A morning blood cortisol test is usually the first step in screening for cortisol disorders.
Normal morning cortisol: 10-20 mcg/dL (micrograms per deciliter)
Normal evening cortisol: 3-7.5 mcg/dL
Levels consistently above 19 mcg/dL in the morning or above 7.5 mcg/dL in the evening may indicate cortisol excess.
Salivary Cortisol Test
Salivary cortisol testing measures the amount of cortisol in your saliva, which reflects free (unbound) cortisol in the blood. This test is particularly useful for detecting Cushing syndrome. A late-night salivary cortisol test (collected around 11 PM to midnight) is highly sensitive for Cushing syndrome because cortisol should be at its lowest at night. Elevated cortisol at midnight is abnormal.
Salivary cortisol is convenient because it can be done at home. Your doctor will give you a collection kit and specific instructions.
24-Hour Urine Cortisol Test
This test measures the total amount of cortisol excreted in your urine over a 24-hour period. It provides the most comprehensive picture of cortisol production and is often used to confirm suspected Cushing syndrome or assess chronic cortisol elevation.
Normal 24-hour urine cortisol: 10-55 mcg/day for adults
Values consistently above 50-55 mcg/day suggest cortisol excess.
| Test Type | What It Measures | When to Use |
|---|---|---|
| Morning Blood Cortisol | Cortisol level at peak time (6-8 AM) | Initial screening for high or low cortisol |
| Late-Night Salivary Cortisol | Free cortisol at lowest point (11 PM-midnight) | Detecting Cushing syndrome |
| 24-Hour Urine Cortisol | Total cortisol excreted over 24 hours | Comprehensive assessment of cortisol production |
Your doctor will choose the appropriate test based on your symptoms, blood pressure control, and suspected cause of cortisol elevation. Multiple tests may be needed to confirm a diagnosis.
Natural Ways to Lower Cortisol and Blood Pressure
If your cortisol levels are elevated due to chronic stress (and not a medical condition like Cushing syndrome), there are several evidence-based strategies to lower cortisol naturally. Reducing cortisol can, in turn, help lower blood pressure.
1. Regular Exercise
Exercise is one of the most effective ways to lower cortisol and blood pressure. Moderate aerobic exercise (like brisk walking, swimming, or cycling) for 30-45 minutes most days of the week reduces baseline cortisol levels by 15-25% and lowers blood pressure by 5-8 mmHg.
Avoid excessive high-intensity exercise, which can temporarily spike cortisol. Balance is key: regular, moderate exercise reduces cortisol, while chronic overtraining can keep it elevated.
For more details, see our article on exercises to lower blood pressure.
2. Prioritize Sleep
Sleep deprivation drives cortisol levels up. Studies show that getting less than 6 hours of sleep per night raises morning cortisol by 45% compared to getting 8 hours. Poor sleep also disrupts the natural cortisol rhythm, keeping levels elevated at night when they should be low.
Aim for 7-9 hours of quality sleep per night. Create a consistent bedtime routine, limit screen time an hour before bed, and keep your bedroom cool and dark.
Learn more about the connection in blood pressure and sleep.
3. Practice Deep Breathing and Meditation
Deep breathing exercises and meditation activate the parasympathetic nervous system (the "rest and digest" branch), which lowers cortisol and blood pressure. Just 5-10 minutes of deep, slow breathing (4 seconds in, 6 seconds out) can reduce cortisol levels and drop blood pressure by 3-5 mmHg within minutes.
Mindfulness meditation practiced for 20-30 minutes daily has been shown to reduce cortisol by 20-30% over 8 weeks. Apps like Headspace, Calm, or Insight Timer can help you build a consistent meditation practice.
4. Ashwagandha Supplementation
Ashwagandha is an adaptogenic herb that has been extensively studied for its ability to lower cortisol and reduce stress. A 2019 randomized, double-blind, placebo-controlled study found that participants taking 125-600 mg of ashwagandha daily experienced cortisol reductions of 11-33% after 60 days.
Another 8-week trial reported significant reductions in anxiety, morning cortisol, and blood pressure in adults taking ashwagandha compared to placebo. Ashwagandha appears to work by modulating the hypothalamic-pituitary-adrenal (HPA) axis, the body's stress response system.
The most commonly studied and effective forms are KSM-66 and Sensoril, both standardized ashwagandha root extracts. Typical doses range from 250-600 mg per day, taken in one or two divided doses.
5. Omega-3 Fatty Acids
Omega-3 fatty acids (found in fatty fish like salmon, mackerel, and sardines, or in fish oil supplements) help reduce cortisol and inflammation. Studies show that omega-3 supplementation (1-2 grams of EPA and DHA daily) lowers cortisol response to stress and reduces blood pressure by 2-4 mmHg.
Aim for 2-3 servings of fatty fish per week, or take a high-quality fish oil supplement. Plant-based omega-3 sources like walnuts, chia seeds, and flaxseeds also provide benefits but are less potent than marine omega-3s.
6. Reduce Caffeine Intake
High caffeine consumption (more than 3-4 cups of coffee per day) can raise cortisol levels, especially in people who are sensitive to caffeine. If you notice that coffee makes you feel jittery or anxious, or if your blood pressure spikes after drinking it, consider cutting back to 1-2 cups per day or switching to decaf.
Read more in our guide on does coffee raise blood pressure.
7. Spend Time in Nature and with Loved Ones
Social connection and time spent outdoors are powerful cortisol reducers. Studies show that spending 20-30 minutes in a natural setting (a park, forest, or beach) lowers cortisol by 20-30%. Similarly, positive social interactions and laughter reduce cortisol and improve cardiovascular health.
Make time for activities that bring you joy and relaxation, whether that is a walk in the park, playing with a pet, or having dinner with friends.
When to See a Doctor
If you have high blood pressure that is difficult to control with lifestyle changes and medications, or if you have symptoms of Cushing syndrome (rapid weight gain, easy bruising, muscle weakness, mood changes), see your doctor and ask about cortisol testing.
You should also see a doctor if you have:
- Blood pressure that remains elevated despite taking multiple blood pressure medications
- Sudden onset of high blood pressure, especially if you are young (under 40) or previously had normal blood pressure
- Symptoms of Cushing syndrome (moon face, buffalo hump, purple stretch marks, severe fatigue)
- Chronic stress, anxiety, or sleep problems affecting your quality of life
Your doctor can order cortisol testing and help determine whether your cortisol levels are contributing to your high blood pressure. If Cushing syndrome is diagnosed, treatment options include surgery to remove a tumor, radiation therapy, or medications to block cortisol production.
Tracking Blood Pressure and Managing Stress
Understanding the link between cortisol and blood pressure highlights the importance of stress management in cardiovascular health. Tracking your blood pressure regularly can help you see how stress reduction efforts impact your numbers over time.
Cardilog makes it easy to log your blood pressure, track trends, and identify patterns related to stress, sleep, and lifestyle changes. By keeping a detailed record, you can work with your doctor to develop a comprehensive plan that addresses both blood pressure and cortisol levels.
Final Thoughts
Cortisol is a powerful hormone that plays a central role in your body's stress response, but chronic elevation of cortisol comes at a cost. It raises blood pressure, increases cardiovascular risk, and can lead to conditions like Cushing syndrome. Even mild cortisol elevation from everyday stress contributes to hypertension and heart disease.
The good news is that cortisol-related hypertension is often reversible. Through consistent stress management, quality sleep, regular exercise, and evidence-based supplements like ashwagandha and omega-3s, you can lower cortisol levels and improve your blood pressure. If you suspect cortisol is affecting your health, talk to your doctor about testing and treatment options.
Taking control of stress is not just about feeling better in the moment. It is about protecting your heart and blood vessels for the long term.